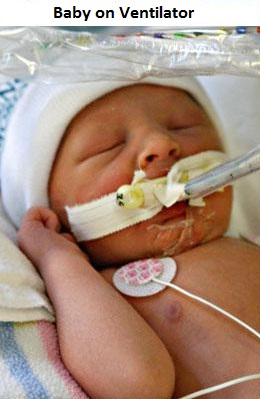
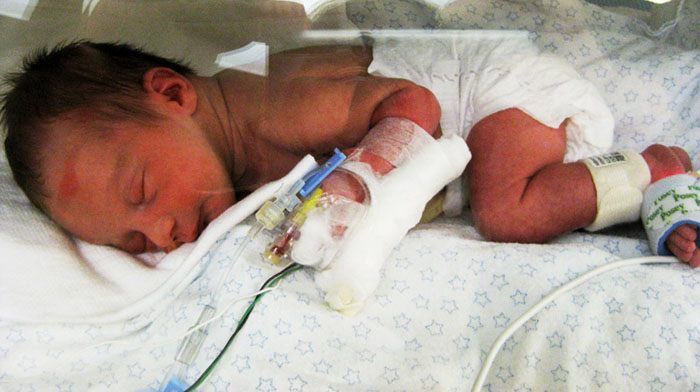
All the tubes and cords hooked up to NICU infants can be intimidating, but they each serve a purpose to help your infant get better. Here is a closer look at some common instruments used in the NICU.
|
A ventilator is used to provide breathing support for ill or immature babies. Sick or premature babies are often too weak, sick, or immature to breathe well enough on their own. They may need assistance from a ventilator to provide "good air" (oxygen) to the lungs and to remove "bad" exhaled air (carbon dioxide). A ventilator is a bedside machine. It is attached to the breathing tube that is placed into the windpipe (trachea) of sick babies who need help breathing.1 |
|
A feeding tube is a small, soft, plastic tube placed through the nose (NG) or mouth (OG) into the stomach. These tubes are used to provide feedings and medications into the stomach until the baby can take food by mouth.
Feeding from the breast or bottle requires strength and coordination. Sick or premature babies may not be able to suck or swallow well enough to bottle or breastfeed. Tube (gavage) feedings allow the baby to get some or all of their feeding into the stomach. This is the most efficient and safest way to provide good nutrition. Oral medicines can also be given through the tube. A feeding tube is gently placed through the nose or mouth into the stomach. It is most often taped in place. An x-ray can confirm correct placement. In babies with feeding problems, the tip of the tube may be placed past the stomach into the small intestine. This provides slower, continuous feedings.2 |
|
This is an oxygen monitor on the infants right foot. The sensor is put on your child's hand or foot and then it is plugged into a machine to read the levels, it has a small red light on one side and a detector on the other side. The red light shines through your child's hand or foot and is seen by the detector on the other side. The detector measures the amount of oxygen in the blood.3 |
|
This is a picture of a NICU infant with an IV in the left hand. IV's are typically placed in the hand, the scalp veins, the feet or they could even be done through the umbilical cord if it isn't dried up yet. Your baby will be able to receive fluids and if needed antibiotics or
"sugar water" to keep up blood sugar and other fluids needed for their care in the NICU. The needle portion of the IV is removed quickly after inserting the IV, so the only part left in the hand is a small rubbery tube that is flexible. The IV is taped to the hand to hold it in place. In the picture to the right the infant also has what is called an arm board. This just helps keep the arm straight so that the tiny tube in their hand doesn't get kinked and the fluids can flow easier. It also helps stabilize the IV so that it won't come out. |
 www.health.vic.gov.au
www.health.vic.gov.au
This infant has heart monitors on its chest which allow the health care workers to monitor the heart rate and respiratory rate of your baby. There may be a few of them to allow for better reading. Infants that are born prematurely are more likely to have heart issues later on, as a result they must be monitored carefully. 4
 flickrhivemind.net
flickrhivemind.net
Some infants may struggle to keep a stable temperature, so a temperature probe, which is like a sticker is placed on their skin, usually in the abdomen area. The infant to the right has a probe placed on the upper abdomen, the wire then goes to a machine which constantly monitors the temperature. It is important to maintain a stable body temperature in infants, so this will help the health care providers know if they need to place your infant under a warmer or use other devices to stabilize their temperature.
Resources:
1. http://www.nlm.nih.gov/medlineplus/ency/article/007240.htm
2. http://www.nlm.nih.gov/medlineplus/ency/article/007235.htm
3. http://www.aboutkidshealth.ca/en/resourcecentres/congenitalheartconditions/understandingdiagnosis/diagnosticprocedures/pages/oxygen-saturation-monitoring.aspx
4. Naulaers, G., Daniels, H., Allegaert, K., Rayyan, M., Debeer, A., & Devlieger, H. (2007). Cardiorespiratory events recorded on home monitors: the effect of prematurity on later serious events. Acta Paediatrica, 96(2), 195-198. doi:10.1111/j.1651-2227.2007.00019.x
1. http://www.nlm.nih.gov/medlineplus/ency/article/007240.htm
2. http://www.nlm.nih.gov/medlineplus/ency/article/007235.htm
3. http://www.aboutkidshealth.ca/en/resourcecentres/congenitalheartconditions/understandingdiagnosis/diagnosticprocedures/pages/oxygen-saturation-monitoring.aspx
4. Naulaers, G., Daniels, H., Allegaert, K., Rayyan, M., Debeer, A., & Devlieger, H. (2007). Cardiorespiratory events recorded on home monitors: the effect of prematurity on later serious events. Acta Paediatrica, 96(2), 195-198. doi:10.1111/j.1651-2227.2007.00019.x